Bruxism Alexandria
Teeth Grinding Treatment in Alexandria
Bruxism is the para-functional grinding or clenching of teeth in involuntary rhythmic or spasmodic non-functional action that are different from normal functional activities like chewing, speaking and swallowing. Bruxism can occur while awake (AB) or during sleep (SB).
SB has been associated with the “arousal response” which is a sudden change in the depth of the sleep during which the individual either arrives in a lighter sleep stage or actually wakes up. Such a response is accompanied by:
- gross body movements
- increased heart rate
- respiratory changes
- and increased muscle activity.
Macaluso et al. in their study showed 86% of bruxism episodes were associated with arousal response along with involuntary leg movements.
Does sleep apnea or airway patency effect bruxism?
According to Spear and others bruxism results from the micro-arousal of the sympathetic nervous system which triggers an increased brain activity, heart rate, respiratory rate, and eventually rhythmic masticatory muscle activity (RMMA’s) resulting in the individual rhythmically closing and grinding of teeth.
The initiation of the micro-arousals has been associated with sleep apnea because bruxism is thought to be the body’s mechanism for opening the airway and increasing oxygenation. Also, additional evidence of the role airway plays in childhood bruxism can be inferred from children diagnosed with sleep apnea.
When their tonsils and adenoids were removed, a 45.6% to 11.8% reduction in the incidence of bruxism was noted following surgery.
The incidence of SB decreases with age from 14-20% in children 11 and younger, to 13% among young adults from 18-29 years of age, to 3% among adults over 60. On the contrary, AB rises from 12% in children to 20% in adults. The average force applied during SB is less than half what can be applied during AB.
A wiring problem in the brain of bruxers.
According to Shetty, et al., disturbances in the central neurotransmitter system may be involved in the etiology of the bruxism. The direct and indirect pathways of the basal ganglion, a group of five subcortical nuclei that are involved in the coordination of movements may be disturbed in bruxers. The direct output pathway goes directly from the stratum to the thalamus from where afferent signals project to the cerebral cortex.
The indirect pathway passes by several other nuclei before reaching it to the thalamus. If there is imbalance between both the pathways, movement disorders result like Parkinson’s disease. The imbalance occurs with the disturbances in the dopamine mediated transmission of action potential. In case of bruxism there may be an imbalance in both the pathways.
Acute use of dopamine precursors like L-dopa inhibits bruxism activity and chronic long term use of L-dopa results in increased bruxism activity. SSRIs (serotonin reuptake inhibitors) such as Prozac exert an indirect influence on the dopaminergic system and may cause bruxism after long-term use. In such cases, the increase in bruxing activity can be mediated by lowering the dose of the SSRIs or by using Buspirone in addition to the SSRI.
Amphetamine which increases the dopamine concentration by facilitating its release also has been observed to increase bruxism. Nicotine stimulates central dopaminergic activities.
This may explain the finding that cigarette smokers report bruxism two times more than the non-smokers and reports of strong evidence that children exposed to second hand smoke affecting their respiratory system have a much higher incidence of bruxism.
Learn more about bruxism and schedule an appointment today!
Can the way your teeth fit together cause bruxism?
There are two ways that describe how people chew. An easy way to visualize these two ways is to think about of how a rabbit might chew and how a cow might chew.
A rabbit might chew in a chopping pattern, in which the teeth never come into contact except when the mandible closes into position where most teeth meet also known as the intercuspal position. In this position the teeth do not touch each other except when they bite together. A cow, however, has a grinding pattern of chewing in which the mandible has a much broader range of horizontal movements during chewing in which case the teeth contact against each other much more.
The cow chewing pattern pattern is associated with more tooth wear and mobility.
In addition, there are two ways in which teeth can fit together. The first is called maximum intercuspal position (MIP). MIP refers to the occlusal position of the mandible which the cusps of the teeth of both arches fully interpose themselves with the cusps of the teeth of the opposing arch. This position used to be referred to as centric occlusion. MIP is a tooth to tooth position.
The second way that teeth can fit together is called centric occlusion. Centric occlusion is the maxillo-mandibular relationship in which the condyles articulate with the thinnest avascular portion of their respective discs with the complex in the anterior-superior position against the slopes of the articular eminences.
This position is independent of tooth contact. This position is a jaw to jaw position.
The classic theory that occlusal interferences (tooth contacts that keep the jaw from fully seating into centric relation) such as a high restoration or interferences in excursive movements that may trigger grinding behavior has come into question. Belief among clinicians on occlusal interferences is divided as to whether they initiate tooth grinding.
Multiple researchers have intentionally placed interferences in the occlusion to see if they can initiate tooth grinding, and while several negative effects are seen, such as tooth mobility, tooth sensitivity, muscle pain, and sometimes TMD symptoms occur, rarely if ever, does the patient start grinding.
The treatment of the worn dentition
Attrition versus Erosion
Treatment of the worn dentition begins with attempting to identify the cause of the wear as the etiology can have a significant impact on the future prognosis of treatment.
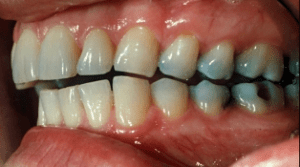
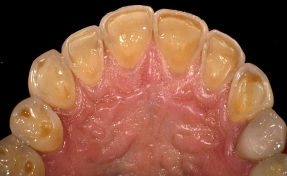
The common causes of tooth wear can be identified as: Attrition, Erosion, Abrasion, and Abfraction. On this page, I have focused on Attrition which is wear on the teeth from opposing tooth contacts on the incisal or occlusal surfaces during mandibular movement.
These movements resulting from bruxism create flat, sharp and shiny wear facets where the teeth have been in contact. In contrast, erosion has cupped rounded area of tooth wear, lacking any flat facets. Of all the causes, attrition has potentially the worst prognosis with the highest risk of future wear or restoration fracture. Attrition is especially dangerous for implant related restorations as they are fused to the bone (lack of a periodontal ligament or PDL).