(TMJ) Temporomandibular Joint Treatment Alexandria
Do you have a TMJ Disorder?
TMJ (temporomandibular joint) disorders are a family of problems related to the muscles of your jaw.
If you are a medical professional, please see the web page: For Professionals->TMJ Disorders .
If you are a patient, answer the following yes/no questions:
- Are you aware of grinding or clenching your teeth?
- Do you wake up with sore, stiff muscles around your jaws?
- Do you have frequent headaches or neck aches?
- Does the pain get worse when you clench your teeth?
- Does stress make your clenching and pain worse?
- Does your jaw click, pop, grate, catch, or lock when you open your mouth?
- Is it difficult or painful to open your mouth, eat, or yawn?
- Have you ever injured your neck, head, or jaws?
- Have you had problems (such as arthritis) with other joints?
- Do you have teeth that no longer touch when you bite?
- Do your teeth meet differently from time to time?
- Is it hard to use your front teeth to bite or tear food?
- Are your teeth sensitive, loose, broken, or worn?
The more times you answered “yes”, the more likely it is that you have a TMJ disorder.
Ready To Improve Your Smile?
What causes a TMJ Disorder?
As described by Howard in Dental Clinics of North America Vol 57 (2013) 99-127, the causes are the following:
- Repetitive strain from playing a wind instrument, a violin, singing, fingernail biting, scuba diving, snorkeling, and swimming
- External blow to the skull as is experienced in an automobile accident, falls, cervical traction, sports injury, intubation, prolonged mouth opening, tooth extraction, and wearing a neck brace
- Hormonal variations (Breighton’s syndrome)
- Stress-related, such as tooth clenching, grinding or tapping
- Teeth grinding at night
- A bite not in harmony with a healthy joint position
- Upper front teeth that do not allow the lower jaw to position itself forward enough
- Upper front teeth that are more than 6mm away from lower front teeth
- Missing teeth
- Inflammatory disorders (including rheumatoid arthritis, juvenile idiopathic arthritis, scleroderma, psoriatic arthritis, ankylosing spondylitis, Reiter syndrome, systemic lupus erythematosus, and gout)
- Infectious arthritis (such as Lyme disease, sexually transmitted disease, gonococcal arthritis, and Chlamydia trachomatis)
- The developmental of an abnormal shape of the head of the lower jaw where it articulates with the skull (such as is seen in a bidif condyle, condylar hyperplasia, or tumors)
- Central nervous system-mediated movement disorders and palsy (such as Parkinson disease, muscular dystrophy, hyperkinesias such as tardive dyskinesia, dystonia, chorea and myoclonus, and palsy such as cerebral palsy and facial palsy)
Diagnosis
Diagnosis begins with a comprehensive examination of the teeth, periodontium (gums), joints, and musculature. If patients present with headaches at their temples (the flattened space on each side of their forehead), pain in front of their ear or on the side of their face, further investigation is necessary to attempt to determine if the cause may be related to the temporal mandibular joints.
Pain from the temporal mandibular joint area can originate from either muscles, joints, or from some other source. Only pain of muscle or joint origin will respond to dental treatment.
The first diagnostic step is to place an appliance similar in appearance to an orthodontic retainer in the patient’s upper jaw. The appliance is called an anterior bite plate (ABP).
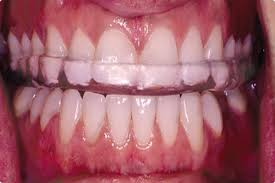
Our usual design choice for the ABP is called a Kois Deprogrammer pictured below.

An ABP significantly reduces muscle activity. It is constructed from a model made of the upper arch and only allows front teeth to touch. Patients who are experiencing muscle pain only often experience pain relief in a little as 24 hours and almost always feel better within a few days.
If the ABP reduces the pain, wearing it at nighttime will be the best approach to managing symptoms. If the ABP increases the pain, likely the joint is involved and the patient will need a second diagnostic appliance.
In such cases, the patient will need a full-coverage appliance (occlusal splint) for long-term wear that supports the joint when the jaw is moved to the side as well as when it is biting straight down.
If neither appliance helps relieve the patient’s pain, it is unlikely that any appliance therapy will be worthwhile, and the patient should consider other treatments such as physical or massage therapy, biofeedback, or muscle relaxants.
It is important to understand before treatment begins that a small percentage of patients only will gain the knowledge that their pain is not related to their muscles or joints and will not receive pain reduction from occlusal treatment.
New to Our Practice?
- Insurance
- New Patients
- Patient Billing
- Patient Registration
- Post Treatment Care
- Restorative Dental Plan
- Schedule an Appointment
Treatment
The initial goals are to relieve the muscle spasm and joint pain. At times this is accomplished with anti-inflammatory medication or a muscle relaxant. In more severe cases, steroids can be injected directly into the joints or muscles to reduce pain and inflammation.
Self-care treatments can often be effective as well and include:
- Resting your jaw
- Keeping your teeth apart when you are not swallowing or eating
- Eating soft foods
- Applying ice and heat
- Exercising your jaw
- Practicing good posture
Treatment often involves the use of a clear plastic appliance known as an occlusal splint pictured below.
An occlusal splint (or nightguard) fits over your top or bottom teeth. As discussed above, different types of appliances are used for different purposes.
An occlusal splint can support your joint and in some cases help you stop clenching or grinding your teeth. Reducing these pathological tooth contacts helps to protect your cartilage and joint surfaces.
An occlusal splint works by removing the influence of your teeth from your chewing system by preventing them from interlocking and reinforcing the position of your existing bite. This allows your lower jaw to relax into a more comfortable position.
Once your bite has adjusted to a new position, Dr. Van Stralen will present options for maintaining your bite in its new, more comfortable position. Those options may involve replacing missing teeth, a bite adjustment (equilibration), orthodontics with or without jaw surgery, or restorative dental work.
Surgical options such as arthroscopy and open joint repair restructuring are sometimes needed but are reserved for severe cases.
Our philosophy is to always consider the most conservative treatment approaches first. TMJ surgery is the last option and is only considered if the jaw joint has pain that cannot be managed in any other way, has severe degeneration, or if the patient has exhausted all other treatment approaches.
Schedule Your Consultation
 If you have some of the symptoms described above and feel that you would benefit from treatment, schedule your consultation today for an evaluation of your TMJ issues and creation of a plan to help you feel better.
If you have some of the symptoms described above and feel that you would benefit from treatment, schedule your consultation today for an evaluation of your TMJ issues and creation of a plan to help you feel better.
Your Teeth Deserve Superior Care
Dr. Van Stralen offers a number of dental treatments that can keep your mouth healthy and your smile beautiful. Contact us today!